In several conversations with different physicians, a question always seems to arise: What can you do to help a patient with lymphedema? Patients and caretakers diagnosed with this chronic condition have asked me the same question. My reply is always the same: “We can do Complete Decongestive Therapy, the gold standard treatment for lymphedema.”
Lymphedema is incurable but can be managed with Complete Decongestive Therapy (CDT), also known as Complex Decongestive Therapy – the gold standard treatment in lymphedema management. CDT is an intensive therapy program consisting of two phases: Phase I-Decongestion and Phase II-Maintenance.
Phase I
The goal in Phase I is to decrease limb swelling and improve skin integrity. There are four components: skincare, manual lymph drainage, compression therapy, and exercises. Skincare is crucial to prevent further skin changes. The products used are acidic soaps and lotions to maintain the low ph that normal skin presents. Manual lymph drainage is a type of light massage that stimulates lymph flow in the lymph vessels and collectors. Compression therapy includes the use of short-stretch bandages along with soft materials such as cotton and foam-based products to create padding and prevent skin breakdown.
Lymphedema exercises include ankle pumps, deep breathing, upper and lower extremity strength, range of motion and functional mobility. Lymphedema patients are recommended to exercise when compression is used in the affected limb to prevent additional lymphatic fluid from accumulating in the interstitial spaces of the skin. Under normal circumstances, blood flow will increase to supply oxygen and nutrients to the working muscle but with lymphedema, this leads to increase swelling. Thus, the patient should exercise while wearing compression bandages or garments.
Phase II
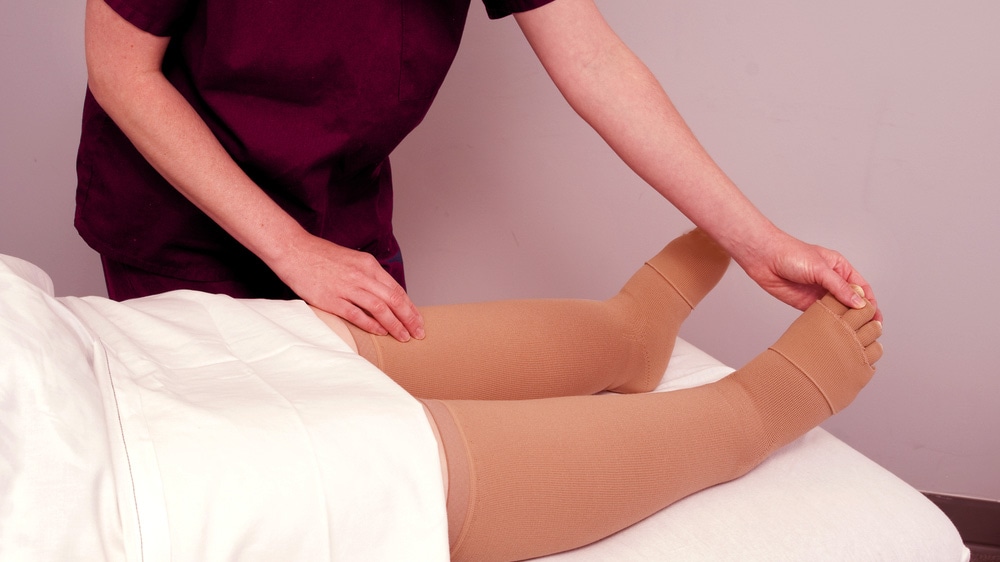
The goal in Phase II is to maintain the limb size achieved during Phase I and prevent exacerbation of swelling. To accomplish this goal, the patient is instructed in skincare, self-MLD, and to wear a special compression garment such as compression stockings or socks and/or velcro wraps. Also, the patient is encouraged to continue with the exercise routine prescribed during Phase I. During Phase II, an intermittent pneumatic compression pump (also known as a lymphedema pump), is recommended. The pump facilitates lymphatic flow but should not be used as a stand-alone treatment but along with the components of CDT.
It is imperative to remark that the patient receiving CDT must be treated by a Certified Lymphedema Therapist or CLT. CLTs have completed specialized training and board certifications to treat lymphedema. Patient safety, limb compromise, circulation problems, skin breakdown, pressure injuries, throbbing pain, the spread of infections, among other complications can arise from untrained individuals performing CDT.
Adherence to the program is necessary for lymphedema management to achieve positive outcomes including the prevention and reoccurrence of swelling. However, it is important to mention that even with good adherence, an exacerbation of comorbidities can lead to re-swelling of the affected limb. Therefore, lymphedema management must include patient education, not only about their lymphedema but their comorbidities as well.
Also, it is our duty as clinicians to advocate for the patient when there are limited resources to manage the patient’s condition. The Florida Breast Cancer Foundation, the National Lymphedema Network, the Academy of Lymphatic Studies, Norton School, and the Lymphology Association of North America (LANA), among others, are available resources for lymphedema management.
Lymphedema doesn’t need to be a debilitating condition. With proper care, education and advocacy, it can be managed. The patient has the right to quality of life and with the help of a Certified Lymphedema Therapist, lymphedema doesn’t have to take that away from them.
References:
- Sleigh, B. & Manna, B. (2020). Lymphedema. Available at: https://www.ncbi.nlm.nih.gov/books/NBK537239/. Accessed January 28, 2020.
- United States Senate Finance Committee Chronic Care Reform. (2015). Available at: https://www.finance.senate.gov/imo/media/doc/Weiss%20Chronic%20Care%20Letter%20to%20Senate%20Committee%20(3).pdf. Accessed January 28, 2020.
- Riches P. (2019) What is Lymphedema? Available at: https://www.medicalnewstoday.com/articles/180919.php. Accessed January 28, 2020.
- Fang-Yih L, Ching-Fu H, & Bai-Yao W. (2012). Elephantiasis nostras verrucosa: swelling with verrucose appearance in lower limbs. Can Fam Physician, 58(10):e551-553. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3470531/. Accessed January 28, 2020.